Reconstitution of hematopoiesis
After transplantation, the donor’s HSC migrate to the bone marrow, where they start to produce the precursors of all hematopoietic lineages. Thereafter, the recipient will have a new hematopoietic system as well as a new immune system of donor origin. By contrast, the non-lymphoid stromal cells in the primary and secondary lymphoid organs will remain of the recipient type. Several factors have influence on reconstitution of hematopoiesis and immunity. EngraftmentGraft take or engraftment (clinically defined as the day that the number of neutrophils surpasses 0.5 G/L) usually occurs between 2 and 3 weeks. Patients with delayed engraftment have a considerably higher risk of complications. Factors that are negatively correlated with early engraftment are GVHD prophylaxis containing methotrexate and a low degree of histocompatibility between patient and donor. Red cells, platelets and cells of innate immunityAs early as 1-2 weeks after transplantation hematopoiesis starts and granulocytes, platelets and erythrocytes appear in the periphery. The newly generated cells are functional but because the initial number is low, the patient needs red cells and platelet transfusions until their counts reach normal range. Read more... T and B cells reconstitution, delayed recovery of immunityEven after the number of cells of most lineages has normalized, the patient may remain immunodeficient for more than 1 year after transplantation. This is mainly due to the malfunctioning of B and T lymphocytes, of which the restauration of functionality is more cumbersome. Read more about T cell reconstitution and about B cell reconstitution. ChimerismMyeloablative conditioning (most frequently used until recently) eradicates the HSC of the patient. As a consequence, the reappearance of recipient cells in these patients is a sign of recurrence of the original disease. In patients who receive a non-myeloablative conditioning, the hematopoiesis may be initially of donor as well as of patient origin (“mixed chimerism”). In some patients, mixed chimerism may be result of the expansion of some recipient T cells having survived the conditioning. Because T cells are long lived, they may persist for several years after transplantation. Read more... |
|
|
Transplantation Immunology | |||||||||||||||||||
|
||||||||||||||||||||
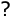

 Print
Print